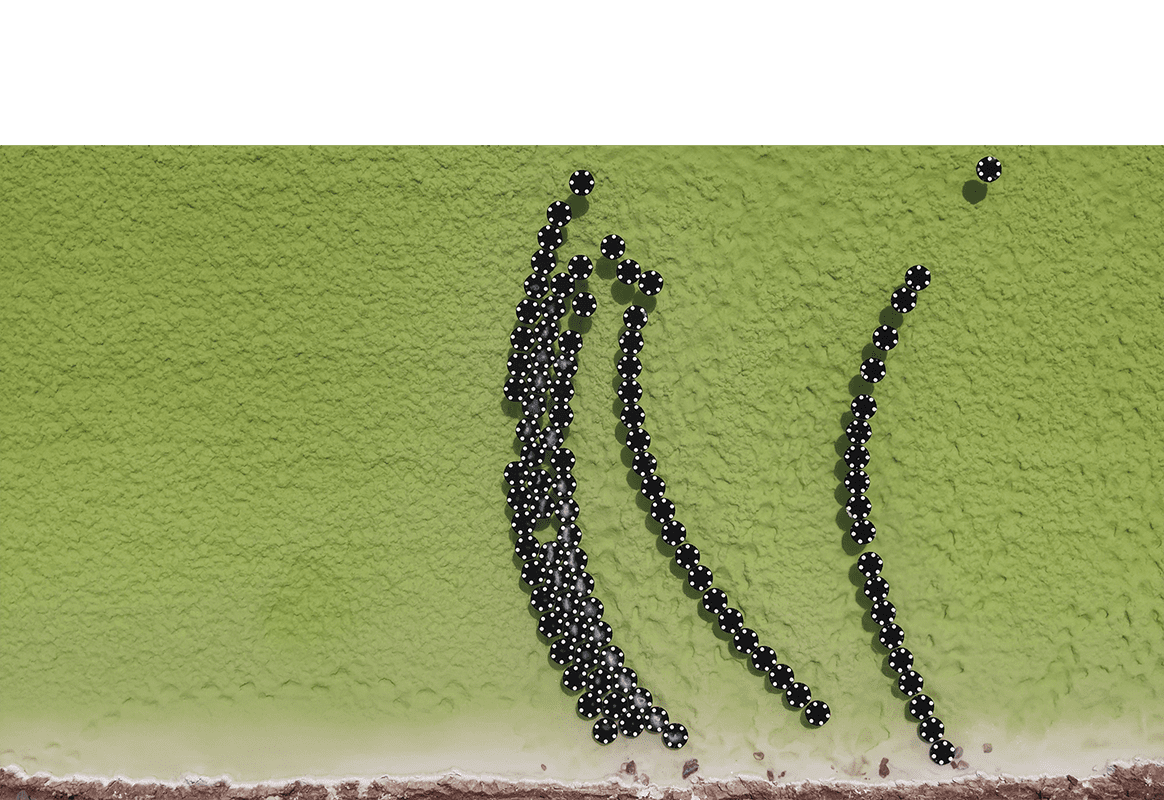Compared to current vaccines, the technology, which relies on a new type of nanoparticle, could introduce five times as much of the vaccine’s active ingredient, mRNA, into recipients’ cells. This technology will be a boon for triggering a stronger immune response while also providing a more scalable vaccine production line, according to Robert Prud’homme, a professor of chemical and biological engineering, and Shahram Hejazi, a faculty member at the Keller Center for Innovation in Engineering Education.
“We had shown that we could encapsulate mRNA prior to the pandemic, but when COVID struck and Pfizer and Moderna said ‘Let’s use mRNA technology for vaccines,’ we said, ‘Ok, with our technology we think we can do an even better job,’” Prud’homme said. “Our technique will allow the delivery of mRNA for COVID at higher loadings than with traditional technology.”
Prud’homme and Hejazi are co-founders of Optimeos Life Sciences Inc., the company developing the new mRNA technology. They started Optimeos in 2016 to bring to market technology developed in Prud’homme’s lab over the last 15 years: inverse flash nanoprecipitation (iFNP), which encapsulates drugs or biological molecules such as peptides, proteins or mRNA in nanoscale particles for more efficient delivery into cells than traditional methods.
Scientists have been pursuing mRNA technology for at least a decade, but with the COVID-19 vaccine rollout, mRNA is suddenly a household term. The mRNA used in Moderna and Pfizer’s vaccines contains genetic instructions for a distinctive feature of the SARS-CoV-2 virus. The mRNA introduces a person’s immune system to this feature, known as the spike protein, allowing their body to produce antibodies that will attack future viral invaders bearing spike proteins.
In addition to thrusting mRNA into the public consciousness, the COVID-19 vaccines have also provided mainstream confidence that these types of vaccines really do work, Prud’homme said. “It’s been spectacular — 95 percent effectiveness is an amazing result.”
There are significant issues with largescale production and distribution of mRNA COVID-19 vaccines. While these challenges are being addressed with the current mRNA vaccines, there is significant room for improvement on the processes and vaccine delivery systems. “We can pack more mRNA into each nanoparticle, and we can easily tune the surfaces of our nanoparticles to better target immune cells,” said Robert Pagels, director of research and development at Optimeos and a 2018 Ph.D. alumnus who studied with Prud’homme. “Taken together, this could mean that lower nanoparticle doses would be needed to elicit an effective immune response, allowing more people to be vaccinated quickly.”
Benjamin Doranz, president and CEO of Integral Molecular, a Philadelphia-based biotechnology company, agrees that Optimeos could provide a solution for many of the challenges still facing mRNA technology — challenges that the pandemic has only laid bare.
“Optimeos’ iFNP technology addresses many of these obstacles, making mRNA production scalable, more efficient and more stable for vaccines and other applications,” said Doranz, who does not have a stake in Optimeos.
Optimeos still has significant research to do before they will be ready to bring a COVID-19 vaccine to market. In December, though, the company received a significant boost when the National Science Foundation awarded it a one-year small business technology transfer grant to develop COVID-19 vaccines using the iFNP platform. In preclinical development, the researchers are using the funding to refine targeted delivery of mRNA to specific types of immune cells and to study the method’s efficacy for mounting an immune response. As Prud’homme said, “This is the proof of concept.”
The Optimeos researchers are also confident that their technology will have applications well beyond the COVID-19 pandemic. In addition to providing a platform for other vaccines, the Optimeos system is well-suited to therapies that would benefit from not eliciting an immune response. Current mRNA-based vaccines contain substances (cationic lipids) that play a role in triggering the immune system. While this is helpful for a vaccine, it prevents application to address medical conditions that require repeated injections. For example, protein replacement therapy for people with a genetic deficiency will require repeated administrations. Other inflammatory diseases fall into this class, said Prud’homme.
“mRNA is the future of medicine, because it’s so specific and so tailored,” Prud’homme said. “It’s really the drug of the future.”